Corneo-scleral topography allows for precise fitting

Scleral contact lenses are now a mainstream specialty lens modality that is embraced by optometry to manage a variety of ocular conditions. Although they are primarily used to fit patients with corneal irregularity,1 especially keratoconus, they also can manage patients with ocular surface disease and high ametropia or astigmatism.
The vast majority of scleral lenses are fit using diagnostic lens fitting sets that are specific to a particular scleral lens design. Diagnostic lens fitting is a trial-and-error process that is inherently inefficient, making lens design more art than science. This is what makes the learning curve steep for the beginner but can challenge even experts with difficult cases. The solution to this cumbersome methodology is to image the anterior ocular surface first, then use measurements to design a custom scleral lens to fit an individual eye.
Topography
Corneal topography instruments have been around for decades, and they have been successfully used to diagnose and monitor corneal disease. They are also used to fit corneal gas-permeable (GP) lenses.
Unfortunately, the keratometry readings from topography are not useful for scleral lens fitting because the vault of a scleral lens is fit based upon sagittal height. Additionally, placido-based corneal topographers are not able to measure out onto the conjunctival/scleral surface, which is necessary to accurately design the geometry of a scleral lens haptic.
Related: Blood-derived serum tears go beyond conventional therapy
Profilometry
The relatively recent development of the first corneo-scleral topographers-instruments that can measure both the cornea and scleral surfaces- is revolutionizing understanding of the shape of the anterior ocular surface and allowing eyecare providers to custom design scleral lenses from measurement.
The sMap3D (Precision Ocular Metrology) corneo-scleral topographer is an instrument that uses triangulation and structured light to measure both the cornea and scleral surfaces, including extreme irregular surfaces that can’t be measured with reflected placido based corneal topographers. The measurements taken with sMap3D have been shown to be repeatable2 and are used to design Europa and Latitude (Visionary Optics) scleral contact lenses.
Related: Year in review of optometric advancements
Taking measurements
The first step for measurement using sMap3D is to instill fluorescein, which is required for the instrument to recognize the clear tissue of the cornea and bulbar conjunctiva. The patient is then positioned and directed to look at a fixation target.
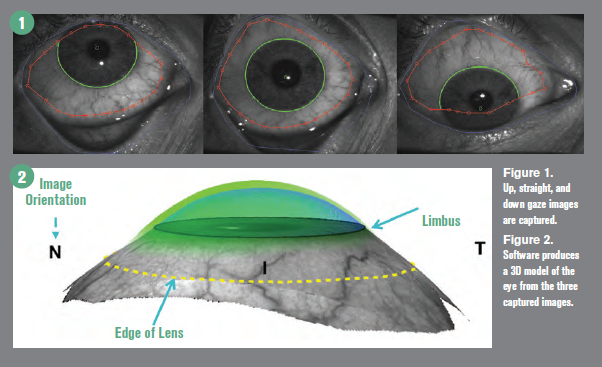
Specific to sMap3D is that three different images of the eye are taken in straight, up, and down gazes (Figure 1) while the lids are retracted. This series of measurements is critical to get data from underneath the lid that can’t be obtained with a straight gaze only measurement.
Research shows that 68 percent of eyes would have less than 50 percent of coverage necessary to fit a 16 mm scleral lens if only the straight gaze measurement is used.3
The three image sets are stitched together using proprietary software that can provide data to 22 mm in diameter 360°, ensuring the ability to fit large scleral lens diameters. A three-dimensional model is produced from the stitched image sets that is used for lens design (Figure 2).
A diagnostic scleral lens is placed on the eye for over-refraction and power determination.
At this stage, the practitioner can send measurements to the contact lens manufacturer for a consultant to design a Europa or Latitude scleral lens.
Europa scleral lens has pre-designed parameters that can be customized, including back surface haptic toricity and quadrant-specific or multi-meridian designs, depending on the scleral shape measured. Precision Lifts can be added to the lens haptic to accommodate pingueculas or conjunctival blebs.
Latitude scleral lens is a free-form custom and contoured lens designed directly from measurement. The lens is ordered directly without the need to adjust the lens curves because there are no pre-designed parameters.
Custom and contoured lenses have been made for several years using application of dental molding materials to the eye (EyePrintPro). I have found the use of sMap3D and Latitude lenses to be easier and more affordable for the patient.
Related: Know the hidden links among glaucoma, contact lenses, and the cornea
Scleral shape
Two recent papers by the Scleral Shape Study Group (SSSG) have studied scleral shape and their findings have a significant impact on modern scleral
lens fitting.
The first of these papers looked at the qualitative assessment of scleral shape patterns for a group of 152 eyes of prospective scleral lens patients.4 The findings of this study determined that scleral shapes have the following patterns: 6 percent sphere, 26 percent toric, and 65 percent asymmetric.
The second paper looked at the correlation of the cornea and sclera for eyes with corneal ectasias. 5 Findings show that eyes with ectasia have asymmetric scleral shapes.
SSSG papers show that the majority of eyes fit with scleral lenses require a scleral lens beyond a toric design for optimal fitting. The advantage of the sMap3D is that it is able to determine quantitative and qualitative scleral shape measurements and use them for individualized lens design.
Related: How to succeed with multifocal contact lenses
Case examples
Case 1. A 58-year old female patient who had previously had radial keratotomy surgery reported for contact lens fitting OD after previously failing in specialty soft contact lenses. Her most recent glasses prescription was:+4.25 -1.50 x 090; 20/20.
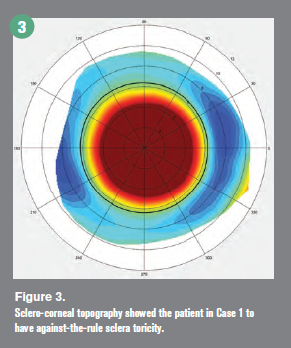
sMap3D corneo-scleral topography revealed her right sclera to have against-the-rule sclera toricity (Figure 3). An additional key finding is that the scleral toricity was symmetric, and a standard back toric design would best fit her ocular surface.
A 16.5 mm Europa scleral lens was ordered with 241 μm of haptic back surface toricity.
Her visual acuity with the scleral lens measured 20/20. The lens demonstrated adequate central corneal clearance and even haptic alignment with no blanching of her bulbar conjunctiva. Topography showed the need for back surface haptic toricity and provided the exact micron amount that would fit the surface of her eye.
Case 2. A 47-year-old female patient had laser-assisted in situ keratomileusis (LASIK) surgery that resulted in corneal irregularity and loss of best-corrected visual acuity with glasses. Refraction OD was +2.25 -2.75 x 165; 20/40. She was originally fit with a back toric scleral contact lens that improved her vision, but she failed due to discomfort.
The patient was measured with the sMap3D scleral topographer. The resultant model identified an asymmetric toric sclera shape with a 300-μm nasal elevation. She was refit with a Latitude scleral contact lens.
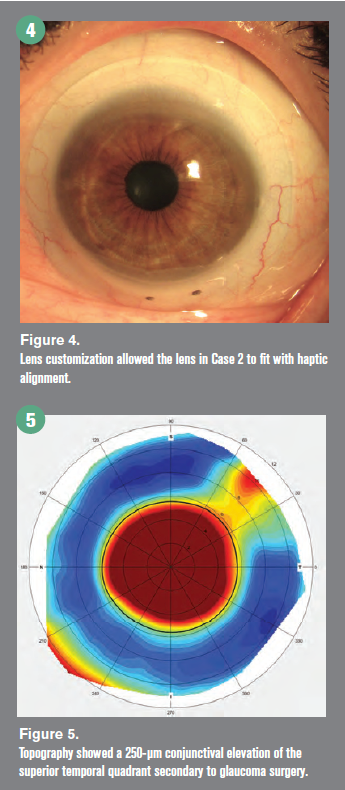
Lens customization to match the conjunctival scleral surface of this eye with significant asymmetry allowed the lens to fit with haptic alignment, demonstrating no compression or impingement (Figure 4).
The Latitude lens improved the patient’s vision to 20/25 and she was, for the first time, able to comfortably wear a scleral lens. It wasn’t possible to determine the best design for this patient until the shape of the sclera was known.
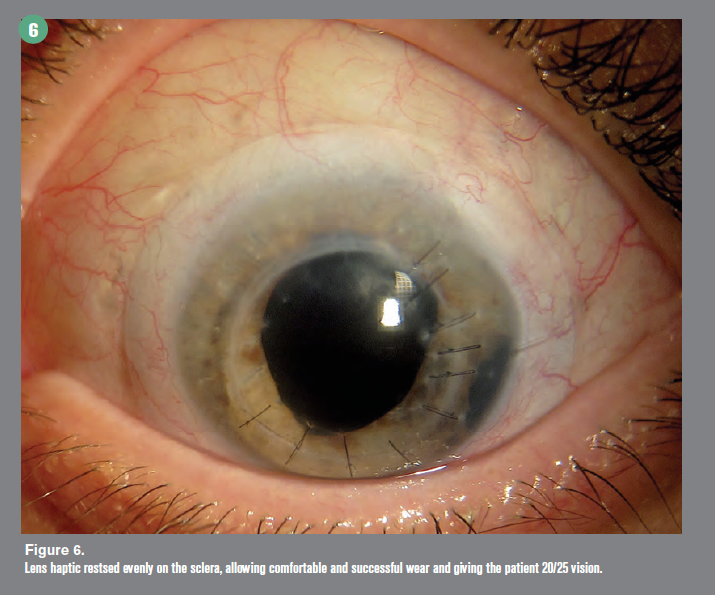
Case 3. A 55-year-old female patient reported for scleral lens fitting OS. She had a history of keratoconus, penetrating keratoplasty, aphakia, and tube shunt surgery for glaucoma. A sMap3D measurement showed 173 μm of scleral toricity. The scleral map additionally measured a 250-μm conjunctival elevation of the superior temporal quadrant secondary to the glaucoma surgery (Figure 5).
A 16-mm Europa scleral lens with back surface toricity and a 200-μm precision lift to vault the elevated conjunctiva was successfully fit. The lens haptic rested evenly on the sclera (Figure 6), allowing comfortable and successful wear, giving the patient 20/25 vision.
The back surface toricity was able to rotationally stabilize the lens so the precision lift was positioned correctly. The lens design was entirely determined using the topography measurement and fitting software. Figure 4. Lens customization allowed the lens in Case 2 to fit with haptic alignment. 4
Related: How the blink affects contact lens wear
Conclusion
The art form of diagnostic lens fitting may someday be obsolete. The future of scleral lens fitting is using metrology measurement for the design of customized scleral contact lenses. The sMap3D is leading the way and revolutionizing corneo-scleral measurement and scleral lens design. The advantage of the fitting customized scleral lenses from the sMap3D results in improved efficiency and success. Ultimately, this decreases chair time and increases profits.
Related: Review clinical highlights of new myopia control lens
References:
1. Shorter E, Harthan J, Nau CB, Barr JT, Hodge DO, Schornack MM. Scleral lenses in the management of corneal irregularity and ocular surface disease. Eye Contact Lens. 2018;46(6):372-378.
2. DeNaeyer G, Sanders DR. sMap3D corneo-scleral topographer repeatability in scleral lens patients. Eye Contact Lens. 2018 Sep;44 Suppl 1:S259-S264.
3. DeNaeyer G, Sanders DR, Farajian TS. Surface coverage with single vs. multiple gaze surface topography to fit scleral lenses. Cont Lens Anterior Eye. 2017Jun;40(3):162-169.
4. DeNaeyer G, Sanders DR, van der Worp E, Jedlicka J, Michaud L, Morrison S. Qualitative assessment of scleral shape patterns using a new wide field ocular surface elevation topographer: The SSSG Study. J Cont Lens Res Sci. 2017;1(1):12-22.
5. DeNaeyer G, Sanders DR, Michaud L, et al. Correlation of corneal and scleral topography in cases with ectasias and normal corneas: The SSSG Study. J Cont Lens Res Sci. 2019;3(1):10-20.
Newsletter
Want more insights like this? Subscribe to Optometry Times and get clinical pearls and practice tips delivered straight to your inbox.